Rewiring Psychiatry: Inside a Bold Push to Transform Mental Health Science
Research into the neuroscience of mental health could help create personalized approaches and more effective treatments.
By Emily Ayshford
For centuries, physicians have tested whether physical interventions could cure mental illness. Most of these interventions failed, however, and were replaced with the current standard of treatment: medications and therapy. That’s because many of the biological underpinnings of mental health still remain a mystery.
At Northwestern’s Feinberg School of Medicine, an invigorated Department of Psychiatry and Behavioral Sciences is working to change that. By using the latest imaging and neurotechnology, the department’s faculty hope to uncover the neuroscience underlying mental illness.
“If we understand the fundamental pathophysiology of psychiatric disorders, then we could develop better treatments that could be personalized for each disease subtype,” said Sachin Patel, MD, PhD, chair of the department and the Lizzie Gilman Professor of Psychiatry and Behavioral Sciences.
Bolstered by philanthropic gifts and a growing faculty team, the department is starting to see promising results. With a push toward implementation science, the team hopes their work can be used to improve treatment outcomes around the world.
Understanding the Biology of Mental Illness
When Patel arrived at Feinberg in 2022 and was charged with reinvigorating the department’s education and research missions, it was a unique moment in history. Many people were feeling the psychological fallout of the COVID-19 pandemic and talking about mental health concerns — including anxiety, depression, and post-traumatic stress disorder — had become more mainstream.
In fact, more than one in five adults suffers from mental illness, according to the National Alliance on Mental Health. And while many have found relief in medication and therapy, a significant percentage do not respond to treatment, including about 30 percent of people with major depressive disorder.
Faced with these statistics and compelled to make a difference, Patel moved to action. First, he recruited new clinician-educators to mentor residents and postdoctoral fellows to improve clinical education. Northwestern Medicine expanded its services, adding an acute observation unit that now provides emergency psychiatric services from emergency psychiatry specialty-trained faculty seven days a week. In addition, the outpatient clinic now offers more same-day treatment services for patients, as the length of untreated illness is a major problem within the field.

Patel also recruited faculty to conduct fundamental brain science research related to mental health — a move that was supported by a generous gift from Stephen M. Stahl, ’75 MD, PhD, DMedSci (Hon.), DSci (Hon.), and his wife Shakila, to launch the Stephen M. Stahl Center for Psychiatric Neuroscience at Feinberg School of Medicine. In November, thanks to a transformative gift from Kent and Liz Dauten and the Dauten Family Foundation, Northwestern Medicine established the Northwestern Medicine Dauten Behavioral Health Institute, a pioneering initiative aimed at redefining behavioral healthcare across Chicagoland and beyond. The new institute also supports the formation of the Bipolar Disorder Center of Excellence.
“Our goal is to become a nationally recognized department of psychiatry that is focused on innovative discovery in mental health that ultimately impacts our understanding of the biology of mental illness and also improves treatment outcomes through discovery of novel interventions and treatment modalities,” Patel said.
Recording Neuron Activity to Understand Mental Health Disorders
Understanding the biology behind mental illness is no small feat. Over 50 years ago, scientists began to remove certain parts of rodent brains and found that when they did so, it affected certain emotions, like fear.
“But as technology became more advanced, scientists realized that in these regions, there is more than one cell type,” said Hao Li, PhD, assistant professor of Psychiatry and Behavioral Sciences and of Neuroscience. “And these cells express different genes. They also often drive the opposite behavior. So, it was much more complicated than having one emotion in one area.”
With 86 billion neurons forming more than 100 trillion synapses, the human brain is a complex network of thoughts, emotions, and memories. But armed with the latest technology, Li is working to understand which cells impact certain behaviors that underlie mental illness.
In his lab, he studies how neural activity corresponds to mice feeling either pleasure from a reward or fear of punishment. To find out, he uses tiny probes that detect electrical activity within certain neurons. He also uses a special lens to record calcium activity in mouse brains. Calcium rises when neurons fire, so Li and his students inject a protein into the brain that fluoresces when calcium rises. That way, they can watch neural activity on a computer screen and correlate it with behavior. “It looks like a Christmas tree lighting up,” Li said.
The goal is to understand how different neuron subtypes communicate with other brain regions when animals encounter reward or punishment. “In many mental illnesses, there is dysregulation in the basic processing of reward and punishment,” Li explained. “People either value being rewarded too much or fear too much. So, if we can understand these basic neural circuits, we can understand how they become dysregulated in mental health disorders.”
If scientists could better understand these cells and their connections, they could ultimately create treatments that better manipulate these neural circuits. “Our work is laying the groundwork for that next step,” Li said.
Creating a Model of How Treatment Affects the Brain
In fact, treatments that physically modulate populations of neurons do exist, and show promising results for some patients. Faculty like Ivan Alekseichuk, PhD, assistant professor of Psychiatry and Behavioral Sciences, are working to understand just exactly how they work — with the goal of creating personalized treatments.
Alekseichuk uses transcranial magnetic stimulation (TMS) to treat patients with depression. TMS uses magnetic pulses to stimulate nerve cells in the brain, a process that has proved both safe and effective for people with depression. Response rates for the treatment can be as high as 70 percent.
Despite the treatment’s success, some patients still do not respond. To better understand why — and to create precise, personalized stimulation — Alekseichuk records the electrical activity within his human patients’ brains as they undergo the treatment.
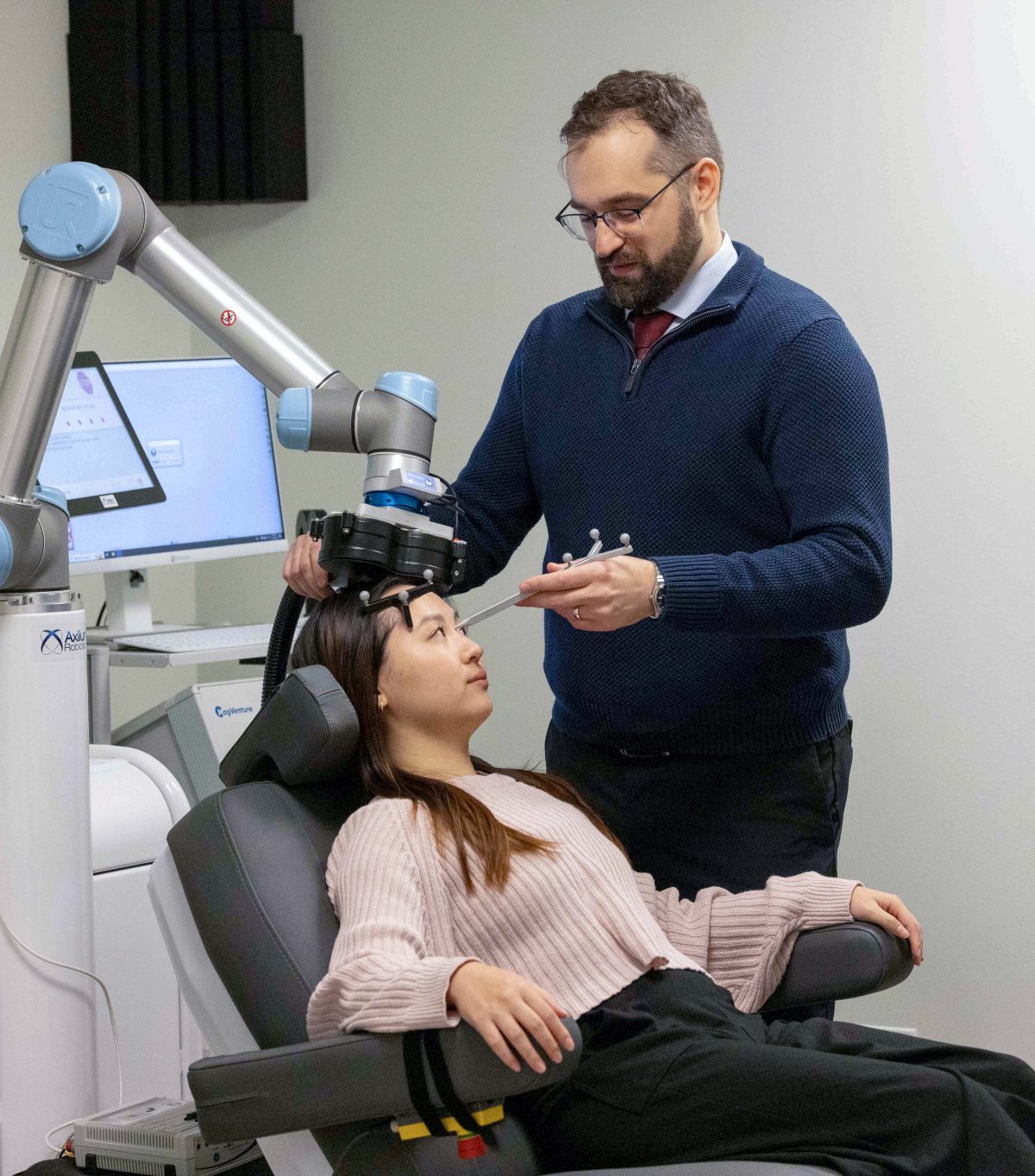
During clinical trials in Alekseichuk’s lab, patients wear sensors around their heads and sit in a chair with a magnetic coil placed close to their scalps. The coil sends repetitive magnetic pulses to the left prefrontal cortex, an area responsible for mood regulation. Those pulses excite the neurons that malfunction in patients with depressive disorder, creating new patterns that propagate throughout the rest of the brain. Alekseichuk and his collaborators use real-time biosignals to track brain states and optimize stimulation. The ultimate goal is to physically measure biomarkers in the brain.
“Right now, to understand if a treatment works, we essentially ask patients how they have felt since the treatment,” Alekseichuk explained. “But we want to use neuroimaging and measures of electrical activity to provide better predictive power about clinical outcomes. We want to characterize mental health disorders not by how people are feeling, but by their biological mechanisms.”
Alekseichuk is using the data from these trials to create virtual simulations of brain activity. This model can help them simulate different scenarios — including different brain structures, dosing, and stimulation locations — to determine which were most effective. “Right now, we’re making sure everyone HAO LI, PHD receives the same treatment, but we have different outcomes,” he said. “We want to find a way to personalize treatments so everyone can have the same outcome.”
Moving Findings Out of the Laboratory
Alekseichuk envisions a future where mental health will be treated like dental care: Patients will have easier access to local practices with highly automated equipment that can provide cost-effective mental health treatments like TMS.
To get to that point, Patel is also pushing for a departmental focus on implementation science. “Even when we know that treatments work, we know that knowledge is often not translated effectively into the clinic and to the people on the front lines of care,” Patel noted. “We want to make our findings in the laboratory broadly accessible to people.”
To reach that frontier, Patel continues to recruit new faculty and work with donors who support the cause. “It’s an exciting time for our field,” he declared. “And the fact that we have so much support from community members and philanthropy speaks to that.”
Revealing Neural Mechanisms Behind Anxiety and PTSD
Led by Sachin Patel, MD, PhD, and the Lizzie Gilman Professor of Psychiatry and Behavioral Sciences, a recent study found that specific cannabinoids produced by the human body may help to quell excessive fear responses in people with post-traumatic stress disorder and anxiety.
The research, published in the Journal of Clinical Investigation, found that mice that had depleted levels of cannabinoid 2-AG, a ligand that’s part of the body’s neurotransmitter release regulation system, had increased fear responses. The findings highlight the key role endocannabinoids play in regulating fear responses and identify 2-AG as a potential target for anxiety therapies.
In a separate study, a multi-institutional team of investigators discovered that targeting a specific neural circuit through noninvasive neuromodulation may help reduce symptoms in patients with post-traumatic stress disorder (PTSD).
Co-author Jordan Grafman, PhD, professor of Physical Medicine and Rehabilitation and of Psychiatry and Behavioral Sciences and director of Brain Injury Research at the Shirley Ryan AbilityLab, found that in 20 participants who received transcranial magnetic stimulation, scientists demonstrated a reduction in functional connectivity within the identified neural circuit and a reduction in PTSD-related symptoms. The results were published in Nature Neuroscience.
Philanthropic Gifts Transform Mental Health Research at Northwestern
In 2024, prominent physician Stephen M. Stahl, ’75 MD, PhD, DMedSci (Hon.), DSci (Hon.), and his wife Shakila generously funded the Stephen M. Stahl Center for Psychiatric Neuroscience at the Feinberg School of Medicine.
The center supports investigators across Northwestern who share the common goal of understanding the neural mechanisms underlying illnesses including schizophrenia, bipolar disorder, and post-traumatic stress disorder (PTSD).
“The excitement is that neuroscience has just exploded,” Stahl said. “In the old days, there were only a few targets for medications. Now, what’s happening is that we get to understand the brain and what goes wrong in these illnesses. The future is bright, even in areas like substance abuse, thanks to new experimental animal models helping us to understand it.”
With its $25 million gift from Kent and Liz Dauten and the Dauten Family Foundation, Northwestern Medicine will establish the Northwestern Medicine Dauten Behavioral Health Institute as well as the Bipolar Disorder Center of Excellence, which will be the institute’s first major initiative. The institute aims to lead in delivering superior clinical care, driving novel diagnostic and treatment approaches, and shaping the future of behavioral healthcare nationally, while the center will provide comprehensive, high-quality, patient- and family-centered care and serve as a platform for translational research with a large and defined clinical population and strong neuroscience environment.
“We are honored to support Northwestern Medicine in its mission to elevate behavioral healthcare,” said Liz Dauten, president of the Dauten Family Foundation. “Our family’s philanthropy has prioritized the field of brain science and mental health where there is an explosion in demand for care and an urgent need to find better treatments,” Kent Dauten added. “As long-standing supporters of the Northwestern Medicine three-pronged model — clinical care, research, and education — we could not be more excited about this new collaboration.”
Learn more about Stahl and his contribution to Feinberg and psychiatric neuroscience.










