Care Without Compromise
photography by LAURA BROWN
Adapting to new realities while going the extra mile.
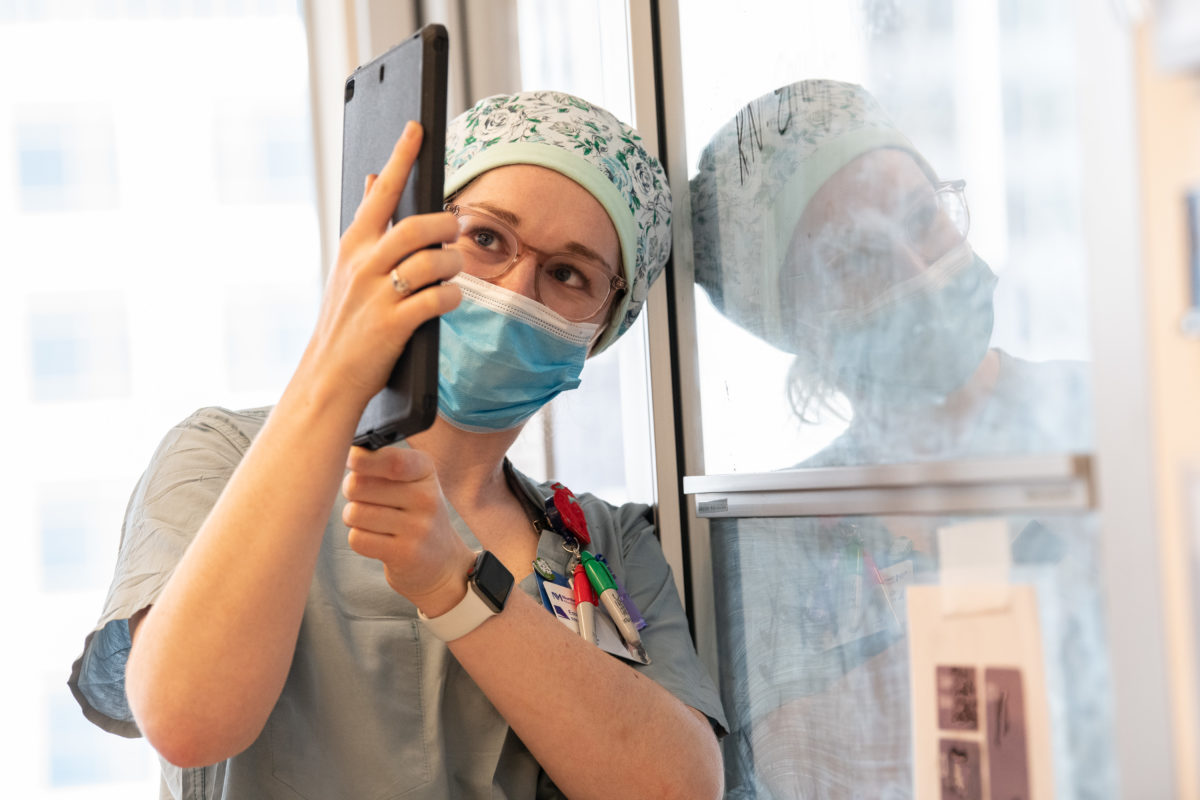
Despite the challenging landscape, a spirit of camaraderie and determination has allowed Northwestern Medicine staff and physicians to overcome many of the unique obstacles presented by the COVID-19 pandemic. Various initiatives and programs were designed in mere days to provide the best possible patient care, whatever the circumstances.
Monitoring COVID-19 patients at home
Northwestern Medicine created the COVID-19 Patient Monitoring Program, which brought together more than 500 individuals, including Northwestern University Feinberg students and Northwestern Medicine staff from a variety of specialties. The program was designed to monitor and support patients who are not hospitalized but who tested positive, have pending results, or are presumed to have COVID-19.
“We identified there was a gap for the patients who were getting this diagnosis and going home,” explains Gayle Kricke, PhD, MSW, director of operations for primary care and an assistant professor of General Internal Medicine and Geriatrics in the Department of Medicine, who was among those to help develop the program with Jeffrey Linder, MD, MPH, chief of General Internal Medicine and Geriatrics. “This presented a unique opportunity to both monitor and advise them.”
Since more than 80 percent of patients with COVID-19 do not require hospitalization, the program offered an efficient process to monitor patients at home and, if necessary, triage them to the appropriate level of care.
It was developed and launched in just four days, a feat made possible by teamwork. “The speed and skill with which leadership, project management, medical students, nurses, advanced practice providers, attending physicians, and information systems staff came together were nothing short of remarkable,” says Linder.
Each day, patients are asked to report their symptoms through NM MyChart. Those who do not respond or who report severe symptoms receive a phone call from a clinician.
“We’re trying to help patients stay at home and be well through their illness, but we’re also keeping an eye out for severe symptoms and patients who need the Emergency Department or hospital-level care,” says Linder.
“We’re helping people remain safe in their home, knowing that someone is checking up on them,” says Kricke. “If they meet certain criteria, we will triage them and do a warm handoff so the ED is aware they are coming.”
This level of care has been made possible by seamless teamwork, and patients benefit. “I just feel so much better when you call,” reported one patient. “Not physically, but emotionally. It’s so nice to get reassurance and to know someone is keeping an eye on me.”
Deploying Surge Staffing
Karl Bilimoria, MD, vice president for quality at Northwestern Memorial HealthCare, and a group of project managers from the Northwestern Medicine Project Management Office coordinated with each hospital’s surge staffing teams to engage physicians in a tiered structure that would meet demand when more patients seek care for COVID-19. Systemwide surveys were rolled out to invite physicians to participate in the COVID-19 surge staffing.
“It was amazing to see how many individuals came forth to help in any way they could,” says Bilimoria, who is the John Benjamin Murphy Professor of Surgery and associate professor of Surgery in the Division of Surgical Oncology and of Medical Social Sciences. “More than 1,700 physicians, advanced practice providers, and trainees responded. This kind of collaboration and support is what makes our health system stronger.”

From Cardiac Medicine Unit to Cardiac ICU in a day
Beginning in mid-March, Jaime Hosler, BSN, CCRN, patient care manager for the Coronary Care Unit at Northwestern Memorial Hospital, was part of the team that made plans for how to best care for patients with COVID-19 while also caring for patients who do not have COVID-19 but who require intensive care.
A plan came together to expand COVID-19 care capabilities by converting the Northwestern Memorial Hospital ninth-floor Galter unit to a COVID-19 unit. That meant staff would have to move the 14-bed Coronary Care Unit from Galter to the eighth floor of the Feinberg Pavilion.
Over just eight hours on a Saturday, Hosler and her team transformed a regular Cardiac Medicine Unit in the Feinberg building into a fully operational Cardiac ICU, with all the necessary monitors, supplies, medications, and equipment. Patients were transferred into the unit the same day.
“All of this work occurred on the same Saturday the patients were moved to the new Cardiac ICU — an incredible amount of work completed within hours,” says Hosler.
To outfit the new COVID-19 ICU, the following work was completed in one day: GE Healthcare helped get ICU monitoring equipment up and running; staff members from the Pharmacy department restocked its shelves and reprogrammed their medication management system; supply carts were built and stocked with ICU equipment and COVID-19 PPE; cameras were installed in patient rooms to allow remote monitoring of patients and limit the number of times nurses had to don PPE to enter the rooms; and the Infection Prevention and Engineering departments created negative airflow for the new rooms.
“The response to this crisis was strategic and comprehensive,” says Hosler. “This work was a true display of teamwork and excellence.”
Emergency Medicine at Its Best
Matthew Kippenhan, MD, medical director of the Emergency Department at Northwestern Memorial Hospital and assistant professor of Emergency Medicine, rose to the challenge of helping his team navigate the pandemic. From putting extra staff in place and making updates in Epic to implementing the rapidly changing PPE and clinical guidelines, Kippenhan says the staff have been very flexible through it all, and he is grateful for the support from everyone at Northwestern Medicine.
“I’ve been absolutely astonished by how much people have really advocated for us,” he says. “Northwestern Medicine Incident Command has been vital to allowing rapid escalation of issues and adjusting hospital capacity. In addition, our physicians, residents, advanced practice providers, nurses, technicians, and Registration and Security team members have been selfless with their time and skills. Despite the rest of the world being on hold, these team members arrive each day ready to tackle any emergency.”
Kippenhan says the outpouring of gratitude from patients has been touching. “I had more patients say thank you in the past few weeks than ever in my career,” he says.

Bringing kidney dialysis home
After surviving three heart transplants, multiple near-fatal infections, and a failed kidney transplant — along with being wheelchair bound due to spending nearly a year in and out of ICU — Lydia Sotomayor, 33, suddenly found herself also having to confront COVID-19.
“I came home in November 2019 after being in the hospital for almost a year, but I was still going to a center for hemodialysis three days a week,” she says. “When the pandemic struck, I was scared. I didn’t want to do that anymore.”
Diseases of the kidney don’t pause for COVID-19. Dialysis patients still need treatment, but hemodialysis centers can have dozens of stations, relatively close together — a risky scenario in a deadly pandemic. Northwestern Medicine has responded by coordinating home dialysis for its most vulnerable patients. Sotomayor, whose kidney and last heart transplants were both conducted at Northwestern Memorial Hospital in 2018, is one of them. (She had her first heart transplant at the age of 15 at Ann & Robert H. Lurie Children’s Hospital of Chicago, then Children’s Memorial Hospital.)
“Within a week of Lydia’s decision to switch to home peritoneal dialysis (PD), our surgeons placed a peritoneal dialysis catheter. Then, she and her mother were trained by our dedicated home dialysis team for almost four weeks,” says her nephrologist, Vikram Aggarwal, MD, assistant professor of Medicine in the Division of Nephrology and Hypertension.
During that time, Sotomayor came to the clinic five days a week for four to five hours each day to train with Leslie Jansto, RN. Normally, patients receiving PD training travel to two different places (a center for hemodialysis and the clinic for PD therapy), but to expedite Sotomayor’s training while keeping her socially distanced, Northwestern Medicine’s home dialysis clinic did both therapies onsite, on a more efficient schedule. The team — which included Lydia, her mom, social workers, nurses, and a dietitian — Aggarwal says, “worked as a family” to get Sotomayor set up to do PD at home.
“I am so grateful,” says Sotomayor, who is now doing just PD at night while she sleeps, no longer risking her health to get to a dialysis center — and enjoying having her days freed up.
“This is one of the most challenging cases of home dialysis training I have seen in my 15 years of practice,” says Aggarwal. “Lydia’s story should be an inspiration for others who want to lead a better quality of life by doing dialysis at home, and the experience of COVID-19 — which has already resulted in a 10 to 20 percent increase in home therapy — will serve as a catalyst for much-needed refinements in home dialysis care delivery.”
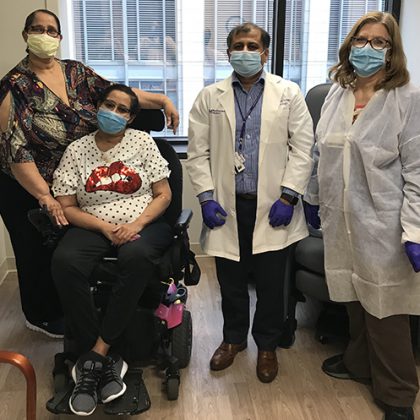
The team worked as a family to get Sotomayor set up to do peritoneal dialysis at home.
Vikram Aggarwal, MD










