Brain, Heart, & Courage
by CHERYL SOOHOO | photography by LINDSEY DECICCO and KIM BECKER
A risky, life-saving brain surgery calls for a novel plan.

On February 4, at 3:02 p.m., cerebrovascular neurosurgeon Babak Jahromi, MD, PhD, sent an e-mail with an unusual request to cardiac electrophysiologist Bradley Knight, MD.
He needed a “heart stopper.”
Five minutes later, Knight, who had never met Jahromi, responded in the affirmative.
A week later, the two were in the operating room, leading a 12-member team performing a rare, life-saving, transvenous embolization on ShaTerrah Cummins, 28, of South Bend, Indiana, who, several months prior, had gone to bed with what she thought was a terrible migraine.
In fact, she had suffered a ruptured arterio-venous malformation (AVM) deep within her brain.
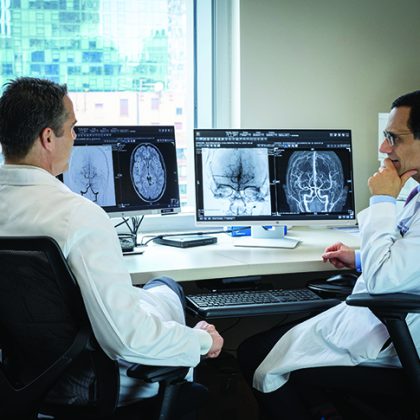
Performing an uncommon embolization technique, Jahromi and Knight forced Cummins’s heart to stop pumping
12 times to reduce blood flow to her brain and help seal her AVM via the use of a special glue-like material. This transvenous, catheter-based strategy was a first for Northwestern Medicine, which now joins only a handful of U.S. medical centers to innovate this bold surgical maneuver.
“We were determined to push the limits to offer ShaTerrah the best therapeutic option,” says Jahromi, who is vice chair of Regional Neurosurgery in the Department of Neurological Surgery and a professor of Neurological Surgery. “The traditional embolization approach is to go through the artery to the AVM. We came from the complete opposite direction — the vein to the AVM. Instead of going downstream, we were going upstream. The procedure required immense expertise and more importantly, a willingness to use our collective skills here at Northwestern to try something we’ve never done before and make it happen.”

A Major Headache
Last September, Cummins had spent her day outside with her two young children. All day, her neck had been killing her. She desperately wanted to crack it for some relief, but feared prompting what she thought were migraines that started when she was pregnant with her now three-year-old daughter.
So she waited for her husband, Christopher, to come home from work. While cooking dinner, she heard the front door open. “I thought, great, now I can pop my neck,” recalls Cummins.
She did and immediately was hit with a severe pounding headache. Taking an over-the-counter pain reliever, Cummins then decided to take a shower.
That was the last thing she remembered before she blacked out.
Her husband found her in their bedroom, where she was vomiting uncontrollably. Thinking his wife needed to sleep off her headache like she had in the past, he put her to bed. The next morning, Cummins could barely speak and needed help walking. After rushing her to the emergency department of a nearby hospital, the Cummins family learned that she had suffered a ruptured AVM. She was quickly transported to a more comprehensive medical center in South Bend, where the clinical team worked to stabilize her by placing a temporary catheter in her brain to drain fluid. After two weeks in the ICU, she returned home — better, but suffering from poor balance, double vision and extreme fatigue. While her AVM had stopped bleeding on its own, the probability of future ruptures was high.
“My options were open brain surgery to take out the AVM, radiotherapy to gradually destroy it with radiation, or to leave the AVM alone — which wasn’t recommended,” says Cummins. “Because my AVM was not in a good place in the middle of my brain and close to the spinal cord, there was a risk of significant side effects with a craniotomy, but my neurosurgeon believed it was the best option. He advised me to get a second opinion and, no matter what, to find the best person for the job.”
Her mother-in-law, a nurse, quickly used her healthcare connections to look for that “best person.” By the end of December, Cummins had an appointment with Northwestern Medicine’s Jahromi, an expert in cerebrovascular diseases with extensive experience in less-invasive endovascular techniques, as well as cerebrovascular surgery.
Brain Plumbing
Plumbing terms come in handy when describing the cardiovascular system, with blood vessels serving as pipes. The largest vessels, arteries take oxygen-rich blood away from the heart to travel throughout the body. Veins do the reverse: they transport deoxygenated blood back to the lungs and heart to be refreshed and recirculated. The smallest blood vessels in the body form capillary beds that allow for the gentle exchange between blood and tissues by controlling blood flow, cell by cell. Usually, the continuous flow of blood through the cardiovascular system works just fine — until it doesn’t, such as in the case of an AVM. Although uncommon (occurring in one per 100,000 adults a year) arteriovenous malformations can be debilitating, if not deadly when they burst.
“Imagine a bowl of angry snakes, with a bunch of pipes going in and out. There is nothing normal about these connections,” says Jahromi, a self-described “brain plumber” who specializes in blood vessels of the cerebrovascular system. “Delicate veins are not designed to handle the high-speed link up to arteries. At some point, that connection is going to burst and then we have bleeding in the brain.”
Cummins had a posterior circulation AVM in what is called the eloquent cortex — a part of the brain that controls vital functions such as speech, movement, and sensation. Removing her AVM through open brain surgery was possible, but presented a substantial surgical challenge: She faced the risk of “collateral damage” and serious side effects ranging from paralysis to cranial nerve injury. Standard endovascular therapy that involves threading a catheter through the groin vessel up to a brain artery to reach the AVM had been ruled out. The snaking architecture of her brain lesion and the fact that the arteries supplying blood to her AVM also supplied normal brain areas made the usual arterial route a no-go.
Looking for other options, Jahromi found one in a single draining vein (versus many) that offered a straight shot to shoot liquid adhesive into the AVM to permanently shut down its blood flow. This anatomical feature of Cummins’s AVM opened the door to a novel transvenous embolization approach. However, Jahromi and his neuroradiology partner, Michael Hurley, MBBChBAO, associate professor of Radiology and Neurological Surgery, would have to inject the glue by atypically going against the current of blood flowing back to the heart. Temporarily stopping the heart from pumping blood to the brain, and consequently preventing it from draining through the venous system, would be essential to the success of this procedure.
For this, they needed a heart stopper.
That’s when Jahromi reached out to a cardiology colleague and asked, “‘Who do you know who could help me with this extremely complex case?’” recalls Jahromi. “He said, ‘Try Brad Knight.’”
We were determined to push the limits to offer ShaTerrah the best therapeutic option.
Babak Jahromi, MD, PhD
Heart Stopper
A cardiac electrophysiologist, the Chester C. and Deborah M. Cooley Distinguished Professor of Cardiology, and a professor of Medicine, Knight sees patients with heart rhythm disorders. In his toolbox is a technique known as cardiac pacing. The minimally-invasive technique involves inserting a catheter through a vein in the leg to the heart to electrically stimulate and artificially manipulate the rate of heart muscle contractions. Somewhat counterintuitively, pacing a heart to a rapid 180 beats reduces blood flow. “The heart can’t beat that fast and effectively eject blood. It just vibrates,” explains Knight. “Yet you can’t pace for too long. The body still needs blood to survive.”
Pacing to stop blood flow usually occurs for no longer than 30 seconds and only one or two times. It is typically employed in cardiac catheterization laboratory procedures involving artificial valve replacement. In Cummins’s case, Knight stopped her heart a record 12 times, for 45 seconds each time, to allow Jahromi a small window of opportunity each time to inject the glue through the vein going against a current that had now been markedly slowed.
“This was a rare scenario and perfect example of multiple specialties coming up with a creative solution,” says Knight. “We applied a technique used for one procedure to a different procedure to make it work.”
The Countdown
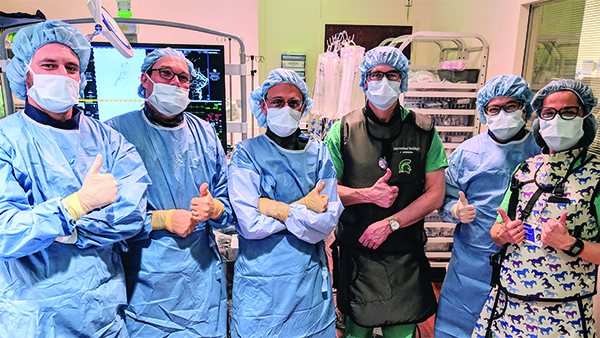
“Four, three, two, one — start pacing.” This critical countdown was the only sound in the room heard at regular intervals during Cummins’s 12-hour procedure. The team kept chit-chat to a minimum. The music that normally plays in the interventional neuroradiology suite had been muted. With their own hearts beating fast, the team brought their A-game. When imaging showed the successful embolization of the AVM, everyone in the room gave each other politely exuberant high fives.
“This procedure was challenging, but it was the least risky option we had before us,” says Jahromi. “ShaTerrah is young and has a long life ahead of her. She deserved a cure, and at Northwestern Medicine, we have a depth of expertise that allowed us to confidently provide her with one.”










